Adopting a gender lens in health systems policy
By Lynda Keeru
Momentum is building towards International Women’s Day marked and celebrated around the world on the 8 March. This indeed coincides with the general international interest among policy makers in knowing what practical steps to take to move towards a more gender-equitable and transformative health system.
This year will also mark 25 years since the Beijing Declaration and Platform for Action adopted at the Fourth World Conference on Women (Beijing, 1995). This conference sought to remove all the obstacles to women’s active participation in all spheres of public and private life through ensuring women a full and equal share in economic, social, cultural and political decision-making.
As the buzz around Universal Health Coverage continues to build, bringing on board the gender lens to policy deliberations cannot be more timely. In this common spirit, a number of advisors and researchers were brought together in Nairobi in February 2019 and developed this guide (Adopting a gender lens in health systems policy: A guide for policy makers) which does a few things:
- Defines what a gender-equitable health system might look like
- Provides a set of benchmarks that health policy makers can work towards
- Features case studies from a range of countries, including Cambodia, Democratic Republic of Congo, Kenya, Liberia, Malawi, Sierra Leone, South Africa, Tanzania and Uganda. These illustrate how decision making that does not take gender into account leads to sub-optimal health systems and provide practical examples of strategies that have been effective in addressing gender barriers in health systems.
- Lists further resources which are accessible online
Gender is everyone’s business

To start with, it is important to note that gender is everyone’s business and not only about women and girls and excluding others as is often misinterpreted. Owing to gender biases, norms, and power relations, some groups of people are often not factored in decision making processes and this means that their needs and rights are not identified, recognized or prioritized.
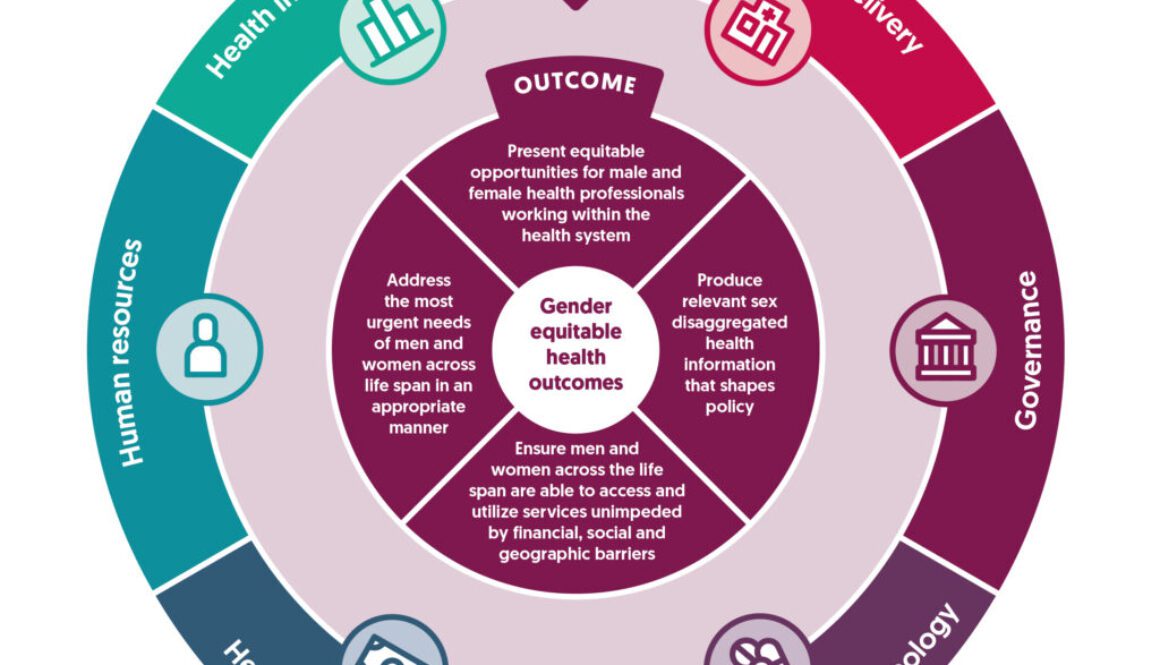
Likening the health system to that of a computer, it has both the hardware and software system. The hardware components include the six building blocks identified by the World Health Organization (WHO). These building blocks include: health service delivery, governance, medical products and technology, health systems financing, human resources and health information systems. The software system on the other hand is hard to see but it is critical as it cements and informs the success of work on the building blocks and includes relationships, values, trust, and power. As the authors in this guide: state: “Both the hardware and software of the health system are affected by gender. Gender norms, roles, and relations are also shaped by the health system.”
The building blocks

On the second page of this very enlightening guide, the authors delve deeply and even graphically into what gender-equitable health systems look like, providing detailed information on the aforementioned six building blocks.
Take for example the importance of providing accessible, acceptable, affordable and available health services as a core function of a health system. Further down that page as you’ll see when you read, there is an illustration of how the divergent needs, rights, access, and experience of health services for men, women, and people of other genders affect the range of demand- (patient-led) and supply-side (health service-led) factors. For instance, a case study from Kibuku district in Uganda demonstrates how health facilities are making life more bearable for physically disabled women.
The second building block is very important as it focuses on health workers who are the backbone of the health system. The policy brief in this section outlines very fundamental recommendations for policy makers based on experience from the different implementers as reflected in the case studies and recommended resources like the WHO (2011) Gender mainstreaming for health managers: a practical approach.
An inclusive health system should, by definition, place fairness and equity at its core. However, many health systems’ governance structures and processes fall short of their potential when it comes to gender equity. There is a lack of goal setting for higher representation of women in leadership and policy spaces in the form of targets, quotas and affirmative action. The guide underscores the key issues in gender and accountability and also suggests ways in which these issues can be addressed by policy makers like ensuring gender balance and gender sensitivity of governance structures at all levels down to the facility and community level.
The brief also features a very well written and interesting case study on “Gender analysis of community health data in Kenya”. It documents the direct impacts of gender on the quality of data reported by Community Health Volunteers due to gendered barriers in data collection. Case in point, what many would regard as a “simple” issue – like the fact that some health issues are perceived to be the domains of men or women – consequently, inform trends like that of Community Health Volunteers collecting data from women. This leads to men’s perspectives missing from the data routinely reported. These gendered elements of data collection impact on dimensions of data quality such as accuracy, completeness, reliability and confidentiality. There’s a wealth of resources put together by the authors of the brief on the same. Check it out!!
‘The phone is my boss and my helper’ – A gender analysis of an mHealth intervention with Health Extension Workers in Southern Ethiopia, mHealth and Gender: Making the Connection and ‘We have the internet in our hands’: Bangladeshi college students’ use of ICTs for health information are some of the works in the brief that have been done by researchers in the area of medical products and technologies and are useful for actors in this field.
Finally, we turn to health financing. This is the accumulation and allocation of funding by and within the health system to ensure service quality and access. As quoted in the guide:
“The extent that financial protection is available to different groups needs to be considered, in addition to how out-of-pocket expenditure is experienced differently by men, women, and people of other genders. This affects policy makers’ ability to deliver Universal Health Coverage.”
Policy makers can give women their rights on International Women’s Day by taking up this recommendation to:
“Ensure that financial protection packages (i.e. prepaid health services under Universal Health Coverage schemes) include essential and routine sexual and reproductive health services, such as childbirth and emergency obstetric care, family planning, cancer care, such as for prostate cancer, and safe abortion.”
Gender mainstreaming is a challenging and ambitious process but we have no choice if we hope to achieve a gender equitable health system and this guide is a gift to all policy makers who are trusted to lead the process.
This guide was developed by Research in Gender and Ethics: Building Stronger Health Systems (RinGs).